GammaCore is also approved for the acute and prophylactic treatment of primary headaches (cluster headache, migraine, hemicrania continua), and reactive airway disease (asthma, exercise- induced bronchospasm, COPD), as well as adjunctive therapy for epilepsy prevention and reducing the symptoms of certain anxiety/depression conditions (eg, panic disorder, posttraumatic stress disorder, major depressive disorder, obsessive- compulsive disorder), gastric mobility disorders, and irritable bowel syndrome
OTHER USES of Transcutaneous Vagus Nerve Stimulation (tVNS):
It is used off label and being investigated (and appears to be effective and safe) for many conditions including:
CARDIAC: Atrial Fibrillation, Heart Failure & MI (heart attack)
HEADACHE: Cluster & Migraine
DEPRESSION
PAIN
TINNITUS (Ringing in the Ears)
STROKE
In our experience, it is effective for Anxiety
(Generalized Anxiety, Panic Disorder and Social Anxiety) and Insomnia.
REFERENCES
Heart
1. Atrial Fibrillation
Chen 2015 Low level tragus nerve stimulation is a non- invasive approach for anti-atrial fibrillation via preventing the loss of connexins
Kapa 2015 Looking Beyond the Ablation Shore, Treating Atrial Fibrillation From Afar
Kreuzer 2012 Transcutaneous Vagus Nerve Stimulation- Retrospective Assessment of Cardiac Safety in a Pilot Study
Li, Shu 2015 2015 Low level non-invasive vagus nerve stimulation- a novel feasible therapeutic approach for atrial fibrillation.
Stavrakis 2015 Low-level transcutaneous electrical vagus nerve stimulation suppresses atrial fibrillation.
Yu 2013 Low-level transcutaneous electrical stimulation of the auricular branch of the vagus nerve- a noninvasive approach to treat the initial phase of atrial fibrillation.
2. Heart Failure
Fan 2010 Transvenous Vagus Nerve Stimulation/ A Potential Heart Failure Therapy Is Feasible In Humans
Wang 2014 Transcutaneous electrical stimulation of auricular branch of vagus nerve- A noninvasive therapeutic approach for post-ischemic heart failure
Wang 2015 Noninvasive vagal nerve stimulation for heart failure- Was it practical or just a stunt?
3. Heart Attack (myocardial infarction)
Wang 2014 Chronic Intermittent Low-Level Transcutaneous Electrical Stimulation of Auricular Branch of Vagus Nerve Improves Left Ventricular Remodeling in Conscious Dogs With Healed Myocardial Infarction
Wang 2014 Low-level transcutaneous electrical stimulation of the auricular branch of vagus nerve ameliorates left ventricular remodeling and dysfunction by downregulation of matrix metalloproteinase 9 and transforming growth factor β1.
Wang 2015 Unilateral low-level transcutaneous electrical vagus nerve stimulation- A novel noninvasive treatment for myocardial infarction.
STROKE
Ay 2015 The effect of transcutaneous vagus nerve stimulation on inflammatory markers in acute stroke
Ay 2016 Transcutaneous Cervical Vagus Nerve Stimulation Ameliorates Acute Ischemic Injury in Rats
Cai 2014 Vagus Nerve Stimulation in Ischemic Stroke- Old Wine in a New Bottle
Capone 2017 Transcutaneous Vagus Nerve Stimulation Combined with Robotic Rehabilitation Improves Upper Limb Function after Stroke
Redgrave 2018 Transcutaneous Auricular Vagus Nerve Stimulation with Concurrent Upper Limb Repetitive Task Practice for Poststroke Motor Recovery- A Pilot Study
Ay 2015 Electrical Stimulation of the Vagus Nerve Dermatome in the External Ear is Protective in Rat Cerebral Ischemia
DEPRESSION
Fang 2015 Transcutaneous Vagus Nerve Stimulation Modulates Default Mode Network in Major Depressive Disorder
Fang 2016 Early cortical biomarkers of longitudinal transcutaneous vagus nerve stimulation treatment success in depression
Fang 2017 Early cortical biomarkers of longitudinal transcutaneous vagus nerve stimulation treatment success in depression
Hein 2013 Auricular transcutaneous electrical nerve stimulation in depressed patients- a randomized controlled pilot study.
Kong 2018 Treating Depression with transcutaneous Auricular vagus Nerve stimulation- state of the Art and Future Perspectives
Li 2018 The effect of transcutaneous auricular vagus nerve stimulation on treatment-resistant depression monitored by resting-state fMRI and MRS- The first case report
Li, Sha 2014 Therapeutic Effect of Vagus Nerve Stimulation on Depressive-Like Behavior, Hyperglycemia and Insulin Receptor Expression in Zucker Fatty Rats
Li, Sha 2014 Transcutaneous Auricular Vagus Nerve Stimulation Triggers Melatonin Secretion and Is Antidepressive in Zucker Diabetic Fatty Rats
Liu 2016 Transcutaneous vagus nerve stimulation modulates amygdala functional connectivity in patients with depression
Polak 2013 Vagus somatosensory evoked potentials are delayed in Alzheimer’s disease, but not in major depression
Rong 2012 Transcutaneous vagus nerve stimulation for the treatment of depression- a study protocol for a double blinded randomized clinical trial.
Rong 2016 Effect of transcutaneous auricular vagus nerve stimulation on major depressive disorder- a nonrandomized controlled pilot study
Trevizol 2015 Transcutaneous vagus nerve stimulation (tVNS) protocol for the treatment of major depressive disorder/ A case study assessing the auricular branch of the vagus nerve
Trevizol 2016 Transcutaneous Vagus Nerve Stimulation (taVNS) for Major Depressive Disorder- an Open Label Proof-of-Concept Trial
Tu 2018 A distinct biomarker of continuous transcutaneous vagus nerve stimulation treatment in major depressive disorder
Wang 2017 Frequency-dependent functional connectivity of the nucleus accumbens during continuous transcutaneous vagus nerve stimulation in major depressive disorder
Yu 2016 Transcutaneous Auricular Vagus Nerve Stimulation/ A Novel Non-Invasive Non-Pharmacologic Treatment for Major Depressive Disorder
please note, in our clinic we have not seen antidepressant effects of tVNS, we do not know why
EPILEPSY (Seizure disorders)
Aihua 2014 A controlled trial of transcutaneous vagus nerve stimulation for the treatment of pharmacoresistant epilepsy.
Barbella 2018 Transcutaneous vagal nerve stimulation (t-VNS)- An adjunctive treatment option for refractory epilepsy
Bauer 2016 Transcutaneous Vagus Nerve Stimulation (tVNS) for Treatment of Drug-Resistant Epilepsy- A Randomized, Double-Blind Clinical Trial (cMPsE02)
DeGiorgio 2013 Neurostimulation for Drug-Resistant Epilepsy
Fischenich 2010 Transcutaneous vagus nerve stimulation- A treatment option in drug resistant epilepsy? (Slides)
He 2009 A new concept of transcutaneous vagus nerve stimulation for epileptic seizure
He 2013 Transcutaneous auricular vagus nerve stimulation as a complementary therapy for pediatric epilepsy- a pilot trial
He 2013 The auriculo-vagal afferent pathway and its role in seizure suppression in rats
He 2015 Transcutaneous auricular vagus nerve stimulation for pediatric epilepsy- study protocol for a randomized controlled trial
Liu 2018 Efficacy and Safety of Treatment with Transcutaneous Vagus Nerve Stimulation in 17 Patients with Refractory Epilepsy Evaluated by Electroencephalogram
Rong 2015 Transcutaneous vagus nerve stimulation for refractory epilepsy- a randomized controlled trial.
Song 2018 A retrospective study of transcutaneous vagus nerve stimulation for poststroke epilepsy
Stefan 2011 First experiences with transcutaneous vagus nerve stimulation (t"VNS) in epilepsy treatment
Stefan 2012 Transcutaneous vagus nerve stimulation (t- VNS) in pharmacoresistant epilepsies/ A proof of concept trial Epilepsia
Yuen 2017 Can natural ways to stimulate the vagus nerve improve seizure control?
HEADACHE
Cluster
Barbanti 2015 Non-invasive vagus nerve stimulation for acute treatment of high-frequency and chronic migraine- an open-label study.
Garcia 2015 Trigeminal sensory nucleus connectivity is modulated by respiratory-gated auricular vagus nerve stimulation in migraine patients
Gaul 2011 Cluster Headache Clinical Features and Therapeutic Options
Gaul 2014 EHMTI-0362. Non-invasive vagus nerve stimulation with gammacore for prevention and acute treatment of chronic cluster headache- report from the extension phase of the preva study
Gaul 2015 Non-invasive vagus nerve stimulation for PREVention and Acute treatment of chronic cluster headache (PREVA)- A randomised controlled study
Gaul 2017 Effects of non-invasive vagus nerve stimulation on attack frequency over time and expanded response rates in patients with chronic cluster headache: a post hoc analysis of the randomised, controlled PREVA study.
Holle-Lee 2014 Noninvasive vagus nerve stimulation in the management of cluster headache/ clinical evidence and practical experience
Kinfe 2013 Partial Response of Intractable Cluster-Tic Syndrome Treated by Cervical non-invasive Vagal Nerve Stimulation
Lavano 2015 Neurostimulation for the Treatment of Cluster Headache
Nesbitt 2015 Initial use of a novel noninvasive vagus nerve stimulator for cluster headache treatment
2. Migraine
Goadsby 2014 Effect of noninvasive vagus nerve stimulation on acute migraine- An open-label pilot study
Grimsrud 2018 Emerging Treatments in Episodic Migraine
Kinfe 2015 Cervical non-invasive vagus nerve stimulation (nVNS) for preventive and acute treatment of episodic and chronic migraine and migraine-associated sleep disturbance- a prospective observational cohort study.
Schoenen 2016 Noninvasive neurostimulation methods for migraine therapy/ The available evidence
Silberstein 2016 Chronic migraine headache prevention with noninvasive vagus nerve stimulation The EVENT study
Straube 2015 Treatment of chronic migraine with transcutaneous stimulation of the auricular branch of the vagal nerve (auricular t-VNS)- a randomized, monocentric clinical trial
3. Other or not specified headaches
Jurgens 2013 Pearls and pitfalls- neurostimulation in headache
h Lambru 2014 Peripheral neurostimulation in primary headaches
Magis 2012 Transcutaneous Vagus Nerve Stimulation (tVNS) for headache prophylaxis/ initial experience
h Martelletti 2013 Neuromodulation of chronic headaches- position statement from the European Headache Federation
Zhu 2016 Non-Invasive Neuromodulation for Headache Disorders
Yuan 2015 Vagus Nerve Stimulation and Headache
Zhu 2016 Non-Invasive Neuromodulation for Headache Disorders
TINNITUS (Ringing in the ears)
Hyvarinen 2014 Transcutaneous Vagus Nerve Stimulation Modulates Tinnitus-Related Beta- and Gamma-Band Activity (EEG)
Kreuzer 2014 Feasibility, Safety and Efficacy of Transcutaneous Vagus Nerve Stimulation in Chronic Tinnitus- An Open Pilot Study
Kreuzer 2014 Feasibility, Safety and Efficacy of Transcutaneous Vagus Nerve Stimulation in Chronic Tinnitus- An Open Pilot Study
Lehtimaki 2013 Transcutaneous vagus nerve stimulation in tinnitus- a pilot study.
Peter 2018 Neuromodulation for tinnitus treatment/ an overview of invasive and non-invasive techniques
Shim Feasibility and Safety of Transcutaneous Vagus Nerve Stimulation Paired with Notched Music Therapy for the Treatment of Chronic Tinnitus
30Hz SUK 2018 Characteristics of Stimulus Intensity in Transcutaneous Vagus Nerve Stimulation for Chronic Tinnitus
Yakunina 2018 BOLD fMRI effects of transcutaneous vagus nerve stimulation in patients with chronic tinnitus
How transcutaneous Vagus Nerve Stimulation Works (Mechanism of Action)
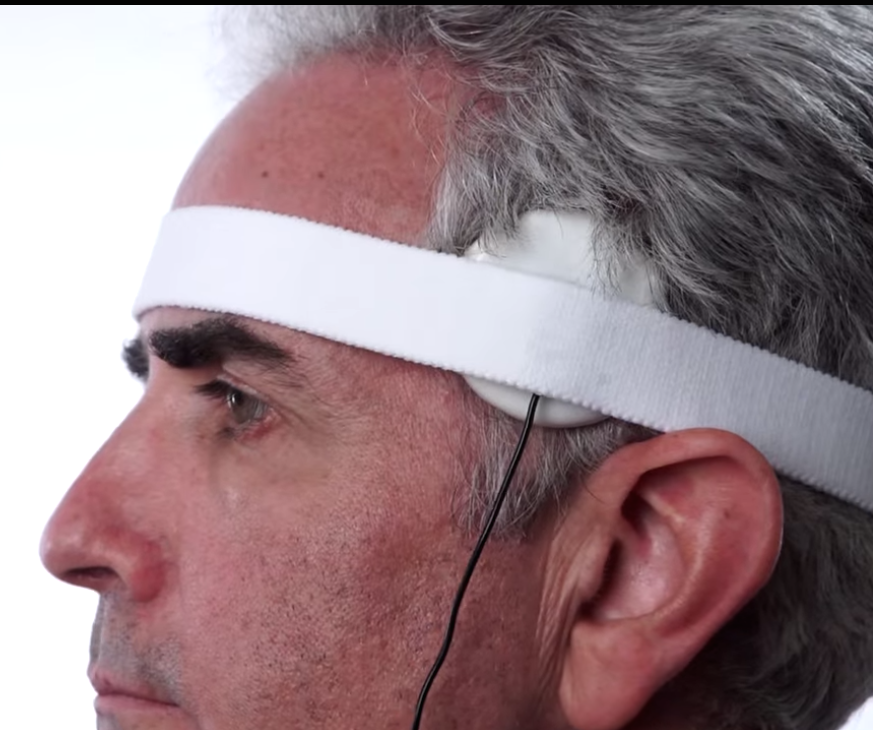
1) stimulating the skin of the ear,
2) stimulates the Auricular Branch of the Vagus Nerve
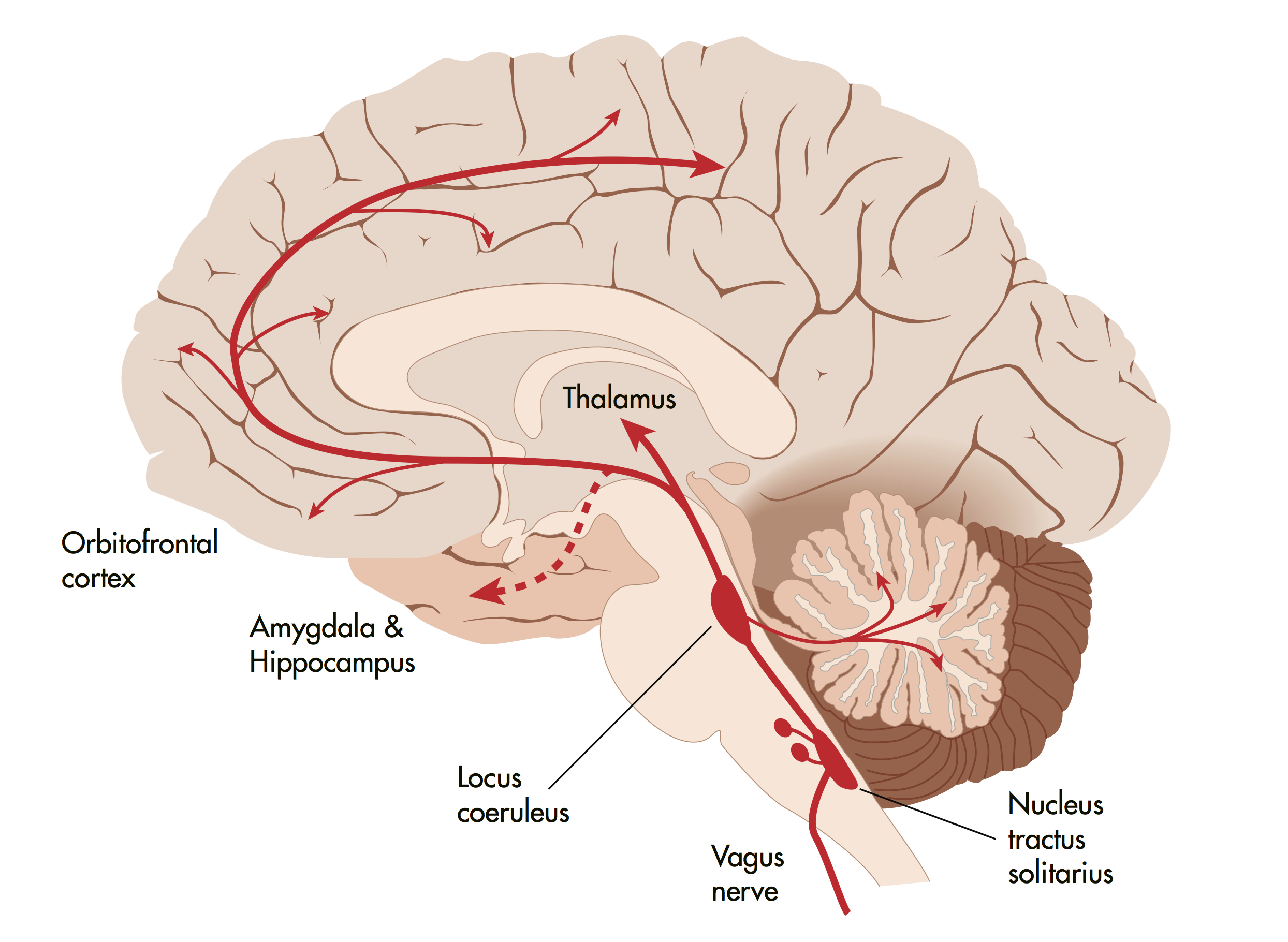
3) the stimulation goes to a nucleus (cluster of nerve cells) called the Nucleus Tractus Solitarius (NTS)
4) the NTS receives information from the body (heart, lungs, intestines, immune system) and
5) sends output to several structures including the Locus coeruleus and indirectly to the Dorsal raphe nucleus.
6) Locus Ceruleus is the brain's primary source of norepinephrine (aka noradrenaline)
7) Dorsal Raphe nucleus is the brain's primary source of serotonin
8) so those two structures influence alertness/energy (norepinephrine) and confidence (serotonin)
9) those two then send those chemicals (neurotransmitters) to the whole brain, especially parts for thinking and feeling. Serotonin (Calm Confidence) & Norepinephrine (Relaxed Energy) - are sent more to the thinking, deliberate, newer Prefrontal Cortex, and less to the Amygdala (Hippocampus and Anterior Thalamus). This reduces anxiety and panic (fight or flight response).
• How Does tVNS Work?